Revenue Cycle Management
- Home
- Revenue Cycle Management
Optimizing Your Practice’s Financial Health with Simplified Billing and Strengthened integrity
In 2014 the revenue cycle management market was valued at $18.3 billion (Ref.: 25 things to know in Revenue Cycle Management, Murphy Brook) and at $260 billion in 2020 (Ref.: Revenue Cycle Management Market Share Report) We will streamline your financial process, reduce overhead administrative costs, no more hiring and training staff, reduction in denied claims, increase in cash-flow, and improved quality patient care.
Managing the revenue cycle in healthcare is complex, involving multiple steps from patient intake to payment collection. At Cosmos Medical Management, we specialize in Revenue Cycle Management (RCM) services designed to streamline your financial operations, improve cash flow, and reduce administrative burdens. Our comprehensive RCM solutions ensure that your practice remains financially healthy, compliant, and efficient.
Our RCM service optimizes each stage of the revenue cycle to ensure timely reimbursements, reduce claim denials, and improve overall financial performance.
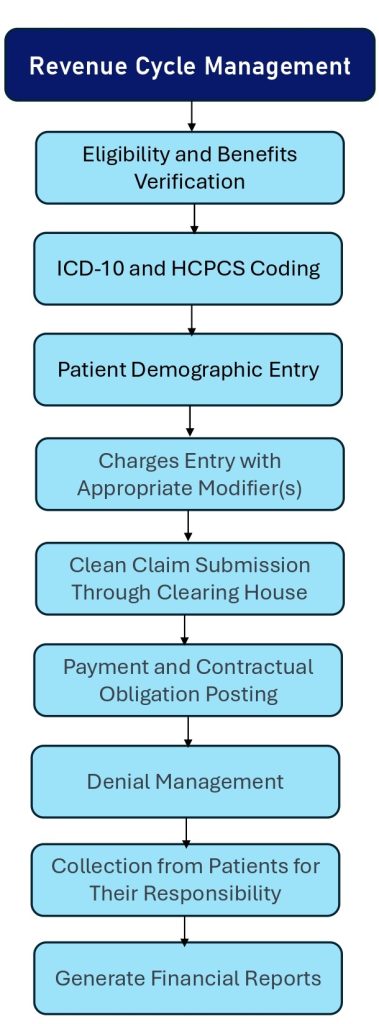
Our Comprehensive RCM Services Includes:
1. Eligibility Verification
2. Charge Capture and Coding
3. Claims Submission and Follow-Up
4. Denial Management and Resolution
5. Payment Posting
6. Patient Billing and Collections
7. Reporting and Analytics
Benefits of Revenue Cycle Management with Cosmos Medical Management
Services
Reach Out to Us Today!
Call Us
Mail Us
Working Time
- M - F: 9:00 am to 6:00pm

Why Choose Cosmos Medical Management for Revenue Cycle Management?
Get in Touch
Contact Us, if you’re ready to optimize your practice’s revenue cycle, reduce claim denials, and improve your financial performance, let Cosmos Medical Management help. Our expert team is here to streamline your RCM process and maximize the financial success of your practice.

Enable healthcare providers to deliver the best care while maximizing their reimbursements by providing an end-to-end solution for Credentialing, Medical Billing, Coding, and Management services.
Contact With Us!
Phone : + 1-918-398-9154
Support Mail : Contact@cosmos-med.com